Reading grim topics like this one is always a tough pill to swallow. No matter the condition, deciding to end your dog’s suffering is a major hit on our psyche and general state of mind.
Health problems that are incurable and have no chance of being reverted can make your dog unrecognizable for owners. Making your mind up if it is worse to have them around in a faded state or euthanize them can often become an increasingly difficult task.
When to euthanize a dog with tracheal collapse depends on several factors, such as the severity of symptoms, response to treatment, and many more elements. This can help you reach the right decision for the dog, even if it hurts you.
Three Signs That Say It Is Time To Say Goodbye

A collapsed trachea is a serious condition that can start chain events that further lower your dog’s life expectancy. Knowing when the dog is in too much pain and under too much stress is important.
The humane thing to do when your dog’s health is severely compromised is to euthanize. Symptoms like coughing, difficulty breathing, and respiratory distress put constant pressure on the immune system.
However, pain causes elevated stress levels, and your dog’s mental health can start degrading too. If vital organs such as the heart or lungs develop conditions following the tracheal collapse, the prognosis will probably not be good.
These next three signs will probably present themselves once it is impossible for the dog to recover successfully, or even if the symptoms are managed, the quality of life will be non-existent. This is when euthanasia should be the only option.
1. Severe Symptoms Overlapping

The first sign that things are not looking good is when various debilitating symptoms occur at the same time, and medication management is no longer an effective way to reduce the strain on the dog’s body.
Most dogs with collapsed trachea exhibit a symptom called honking cough. It is a sound similar to trying to whistle with your lips not fully connected. It is a whizzing sound that is produced when air passes quickly through the small opening between the collapsed walls.
Needless to say, difficulty breathing is another symptom dogs display. The sudden change in lumen diameter makes exhaling hard, but inhaling actually pulls the walls closer together.
This airway obstruction creates a lack of oxygen, and the carbon dioxide accumulates in the lungs, slowly suffocating the dog. Breathing problems intensifying when a dog’s neck is touched are another symptom clearly pointing to a trachea collapse.
A dry cough can often be accompanied by a gagging or retching sound that results in no mucus being expelled. Dogs can get cyanotic or “blue in the face” due to the lack of oxygen in the blood, so bluish gums or burst capillaries in the eyes can be a secondary symptom.
Respiratory distress will occur in dogs with severe cases of tracheal collapse. This is an unsightly image to see, as the dog will violently gasp for air until the collapsed trachea “dislodges” itself to a state that allows for more air to pass through.
2. Heart And Lung Problems
Conditions such as heart failure, hypoxia, and bronchitis are usually present at the same time as the collapse progresses. This is another sign of when to euthanize a dog with tracheal collapse.
Congestive heart failure is defined as the inability of the dog’s heart to properly distribute blood throughout the body. It shares two symptoms with tracheal collapse: difficulty breathing and coughing, but it can aggravate the coughing even if the dog is on antitussives.
The two types, right-sided and left-sided congestive heart failure, have different anatomical issues, but the result is the same — the inability to pump blood to the entire body, which means a severely compromised body condition.
Hypoxia occurs when the tissues and cells do not receive oxygenated blood, leading to organ damage if oxygen therapy is not introduced. However, a dog with a tracheal collapse will share symptoms like difficulty breathing and coughing if the lungs are hypoxic.
Diagnosing hypoxia early can help reverse the potential damage by doing oxygen therapy, but the effectiveness of the therapy will most likely be low due to the dog’s inadequate gas exchange (inhaling and exhaling).
Bronchitis is a condition that has a high chance of developing if your dog has a tracheal collapse. Since inflammation is already present due to the collapse, an already weakened immune system cannot fend off bacterial, viral, or fungal infections. The main symptom of bronchitis is coughing.
This leads to the inflammation spreading into the bronchi and, ultimately, the lungs. Your dog might be too weak to respond to treatment, and in many cases, dogs who are already on anti-inflammatory meds do not respond to antibiotic or antifungal therapy.
All of these serious conditions essentially have the same symptoms that a tracheal collapse has. Because of this, they can be masked as symptoms of only tracheal collapse. If the diagnosis confirms the existence of these conditions, you might want to consider euthanasia.
3. Complete Disinterest

With impeded breathing, your dog will show signs of exercise intolerance, which means a higher chance of obesity. If your dog is refusing to eat food or drink water in addition to exercise intolerance, the lack of nutrients will start a cascading effect of organ shutdown.
Lethargy would be the “next stage” of exercise intolerance. Not only is the dog physically unable to move, but its mental state becomes null.
Many will say that a dog’s state of mind is not as important as the physical one, but in this case, the dog is simply too weak to perform even the most basic and crucial activities, such as eating, drinking, or moving if in pain.
Your dog can give up too. Just like humans, animals know when their body is too weak to recover and simply wait until it is all over. If your dog is non-reactive to sounds or toys in addition to the already mentioned symptoms, then letting go might be the most humane thing you can do.
More On The Trachea, Tracheal Collapse, And Factors That Influence It
Informing yourself about the anatomy of the trachea, the progression of tracheal collapse, treatments, and advice on what you can do to provide some relief to your dog can help you make the difficult decision once it is time.
Visualizing where things are and how they work can be useful in terms of rationalizing why a certain procedure, treatment, or euthanasia is necessary. For starters, let us see how the trachea is built and what its role is.
Anatomy Of The Trachea
As a key part of both the respiratory and digestive tract, the trachea is the conduit that carries air and food into the lungs and stomach, respectively. To understand how a tracheal collapse happens, we need to understand the anatomy behind this organ.
Looking at a cross-section of a canine trachea reveals that it is built out of three layers. The external layer is a connective tissue that hosts tiny capillaries, nerves, and lymphatic channels, and it is called the outer adventitia.
The adventitia also covers the esophagus and gives the organs flexibility. The second layer, called the cartilaginous ring, is the structural reinforcement for the outer adventitia. These are palpable and sometimes even visible in dog breeds with low body fat.
The mucosa is the third and innermost layer, with a crucial role in producing different enzymes that facilitate breathing and proper immune response to pathogens that enter during inhalation or ingestion.
Air humidification occurs with the help of the mucosa, so your dog can properly cool its body through exhalation.
Finally, the Trachealis muscle is made out of smooth muscle tissue, and its primary role is the stabilization of the trachea. It accomplishes that by connecting the ends of the cartilaginous rings, enabling the trachea to contract with the purpose of pathogen expulsion.
This contraction is commonly known as coughing, and the Trachealis muscle, together with the cartilaginous rings, helps the trachea return to its original shape and maintain proper lumen circumference. Lumen is simply a medical term for the inner part of the tracheal “tube”.
What Is A Dog Tracheal Collapse?

Now that we know the main building blocks of the trachea, it will be easier to understand how a tracheal collapse occurs. For the trachea to collapse, several structural elements need to become compromised.
First in line are the cartilage rings. The composition of the cartilage can be weakened by an inherited genetic problem that causes the rings to lose tensile strength and structural integrity.
As the main element in creating and maintaining the round shape of the trachea, the rings bending inwards can cause a collapse which makes the dog have difficulty breathing, let alone eating or drinking.
However, the tracheal rings are not the sole compromised element in dogs with a tracheal collapse. The Trachealis muscle keeps the tension that preserves the shape and gives enough flexibility to the windpipe.
If it becomes loose due to a fault in the tissue or trauma, the rigidness of the entire airway is lost, so inhaling creates a “suction” effect that makes the rings lose structure.
The mucosa walls come in contact (flattening the windpipe and cutting off airflow), leading to a dog’s trachea collapsing.
A Collapsing Trachea Has Four Grades
Higher grade numbers indicate a more severe and advanced tracheal collapse, which means you want to do everything within your power to keep the grade number low.
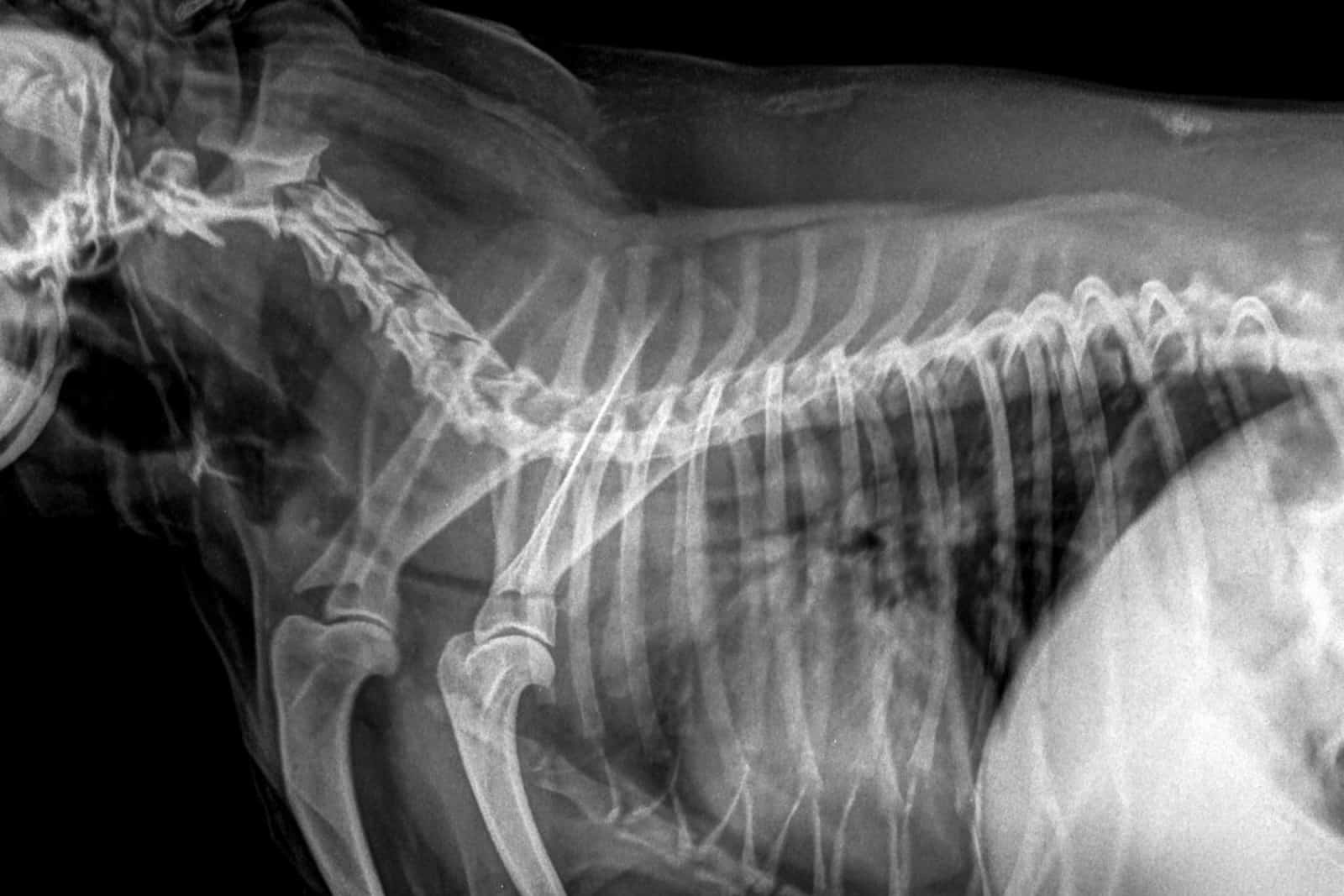
Once the doctor of veterinary medicine does a palpatory test by putting a little pressure on the lower side of the neck, they will diagnose collapsing trachea. In case the symptoms are mild, leading to an ambiguous clinical picture, an X-ray will help clarify things.
- The mildest grade, grade one, is characterized by a slightly loose membrane without major deformity of the cartilage rings. The lumen or diameter of the trachea is reduced by twenty-five percent.
- Grade two of tracheal collapse means that the tracheal membrane is stretched and hanging. The cartilage rings flattening now decreases the tracheal diameter to fifty percent.
- A grade three tracheal collapse will already be a severe case, with the mucus walls (membrane) nearly touching the dorsal trachea. The cartilage rings are almost completely flat, with a lumen reduction of seventy-five percent.
- The onset of nearly full airway obstruction occurs in grade four tracheal collapse, which means that the membrane is completely loose, resting on the back side of the trachea. Cartilage rings are completely flat with the possibility of inversion. Lumen is non-existent.
Grade four tracheal collapse is beyond medical and home treatment, with surgery having a potentially fatal outcome. At that point, the vet will probably discuss with you when to euthanize a dog with tracheal collapse.
Airway Collapse Includes The Bronchi Too
Most cases of tracheal collapse (tracheomalacia) occur in dogs that belong to the small breeds category, but bronchial and tracheal collapse (bronchomalacia) are present in dogs of any size.
The bronchial wall is of a similar composition to the tracheal mucosa (innermost layer). Its main role is to bring air into the lungs, so you can think of them as an “adapter” between the trachea and lungs.
Also known as the conduction zone of the respiratory system, the trachea and bronchi are two indispensable structures for any living being. The collapse of the smooth muscle and interspersed cartilage tissue in the bronchi causes the flattening of the walls.
While the condition anatomically resembles trachea collapse, the symptoms are oftentimes less severe with a more positive prognosis (likelihood of survival with treatment).
A complete airway collapse or bronchomalacia does not have a good prognosis, and, unfortunately, the chance of only bronchial collapse in dogs is low.
Are Some Breeds More Prone To Dog Tracheal Collapse?

Small breeds that have been selectively bred for their “convenient” size and appealing appearance are most prone to tracheal and bronchial collapse.
Most numerous in studies regarding airway and trachea collapse were Poodles or any Poodle crossbreed, Yorkshire Terriers, and mixed breeds involving the Yorkie, Cocker Spaniels, Chihuahuas, Maltese, English Setters, Dalmatians, and the Japanese Spitz.
Small dogs like Toy Poodles, Shih Tzus, and Pomeranians are also high on the list of genetic predispositions to anomalies that can lead to a collapsed trachea.
Other breeds are not immune to tracheal collapse by any means, but these dogs were the recurring candidates used in the analysis of studies, indicating a pattern of genetic predisposition to bronchi and trachea collapse.
Does Age, Sex, Or Physical Condition Matter For Dog Tracheal Collapse?

Although nothing points to tracheal collapses being directly related to the sex of the dog, age does play an important role. This will help you determine when to euthanize a dog with tracheal collapse since an older dog will have a weaker immune system and smaller chances of recovery.
Middle-aged and older dogs are most at risk, especially if they are of one of the breeds listed above. The year span of four to fourteen years of age encompasses both middle-aged and older dog categories.
Another condition that was closely tied to dogs with tracheal collapse is obesity. Because the internal fat tissue (visceral fat) that surrounds organs expands as a dog gains weight, the lungs’ ability to sufficiently expand is reduced.
This makes the process of inhalation and exhalation require more effort, thus becoming fatiguing for the dog. Stale air remains trapped within the lungs, raising the percentage of carbon dioxide without the inflow of fresh air with high oxygen content.
Airflow in the cranial and accessory lobes of the lungs is compromised in dogs with obesity, and infections and inflammation due to hypoxia (reduced gas exchange) can cause secondary and tertiary conditions.
These Things Worsen Symptoms Of Tracheal Collapse
Like any other condition that gets progressively worse without a cure, tracheal collapse requires meticulously planned secondary care. A plan set up by your vet will likely mean a complete lifestyle change for both you and your dog.
Younger dogs suffering from a collapsed trachea will be more difficult to handle because they will have a lot of unspent energy. Physical activity can create massive problems that can quicken the progression of the collapse. This is especially important for high-energy breed dogs.
Living in a humid area or home worsens tracheal collapse symptoms. Dogs will cough more often, putting pressure on an already structurally compromised airway. Even the simplest actions, such as drinking water, can induce dangerous coughing bouts.
Extreme cold or heat can be fatal for a dog with tracheal collapse. High temperatures will cause the dog to overheat without the ability to cool off through exhalation.
Similarly, low temperatures make the air desaturated and harsh. Since the mucosa becomes damaged or not as effective when the trachea collapses, the bronchioles can start dying off due to the air being too dry and cold.
Treatment Options For Dog Tracheal Collapse

Mainly depending on the tracheal collapse grade, your veterinarian will need to rule out other conditions that have similar symptoms. Congestive heart failure can have coughing as a symptom. Cases of both CHF and tracheal collapse present in a dog are not rare.
If your dog coughs without displaying other symptoms and a negative palpation test, your vet will most likely rule out tracheal collapse as the cause.
There are several medical treatment options that include antitussives, corticosteroids, bronchodilators, and sometimes antibiotics. Home treatment usually consists of eliminating activities and external elements that worsen the symptoms.
Surgery is the most serious treatment option, with a long recovery period and a lifetime of medical management to keep inflammation, coughing, possible convulsions, and infection under control.
Medical Treatment
In most cases, this is the treatment that will be necessary for the remainder of your dog’s life, and it will include intravenous or subcutaneous administration of antitussives. Antitussives are cough suppressants that inhibit the activation of the nerve that initializes the reflex.
The strongest form is Butorphanol, and it has a dual purpose — as an analgesic and antitussive medication but is used only in severe cases for simultaneous pain management and cough suppression.
Because it is much stronger than morphine, your dog might be very lethargic and under heavy sedation for the first few days. This therapy is not long-term, and it will be replaced by non-opiate medications if available.
Dextromethorphan is a non-opiate medication that has limited effectiveness in dogs due to its availability and quick elimination from the organism.
Opiate antitussives work best on dogs, so that is the most likely treatment course your veterinarian will take. There is no direct way to treat trachea collapses, and medical management is the best therapy.
Additional Medical Management Therapy
The incessant coughing can create more tissue damage, creating inflammation and opening the possibility of a bacterial infection. This is why some dog tracheal collapses include antibiotic and anti-inflammatory medication.
Corticosteroids are the most commonly prescribed anti-inflammatory meds, with glucocorticoids being the most effective for cough suppression and inflammation due to their strong inhibition of immune responses, such as coughing.
Injections of theophylline are used to expand the blood vessels in the affected bronchi. Theophylline is a bronchodilator, but a more general approach to cough suppression is Benadryl.
The side effects of corticosteroids can include a lowered ability of the body to expedite wound healing, diarrhea, drowsiness, excessive urination, increased appetite, or water consumption.
Cannabidiol, or CBD for short, is an oil that can be given to dogs suffering from tracheal collapse, but its uses are not limited to it. The American Kennel Club has begun a study involving the effects of CBD oil on dogs with epilepsy, so you can expect more information about side effects soon.
Despite being a derivative of hemp, which means no THC compound in CBD, higher doses may cause lethargy or drowsiness, low blood pressure, or dry mouth.
Surgical Treatment
Medical treatment is sometimes not enough to keep the symptoms from completely lowering the dog’s quality of life, which is where surgery comes into play.
There are two surgical procedures for a collapsed trachea — intraluminal tracheal stenting and extraluminal prostheses (rings). Both are quite complex and can only be performed by a board-certified veterinary surgeon.
Dog owners should be aware that these procedures are very costly, and finding a certified surgeon is tougher than you might think. If one is not available in your area, you might have to wait for a long period of time to get an appointment in another city or state.
Both surgical procedures are exclusively done on severe cases of tracheal collapse, meaning grade three and grade four, with a high complication rate.
Extraluminal Prostheses
Since the tracheal rings that are naturally present in the trachea are collapsed at a point in the tracheal tube, polypropylene rings are sutured to the outer part of the trachea and then anchored to the surrounding tissue to stretch the collapsed walls.
While the success rate of this kind of surgery is high and followed by a decrease in displaying symptoms, dogs that have a tracheal collapse in the chest will not be optimal patients for this procedure.
Accessing the chest and suturing the polypropylene rings is impossible without damaging surrounding tissue and organs, so alternative methods are more appropriate for a chest tracheal collapse.
There are complications that can occur after surgery. A high complication rate combined with good survival chances means that most complications are manageable. Pneumonia in dogs occurs due to the extremely weakened immune system after surgery but can be successfully treated.
Tracheal collapse can happen in another segment of the tracheal tube, so fixing one spot might reveal another weak spot. In this case, the prognosis is not good.
It is possible for the implants to fail, meaning that the sutures or tissue break under the tension of the surgical thread. The prognosis, once again, is not favorable for the dog.
Sixty percent of dogs who had a full post-operative recovery within fourteen days live without any medical management, so not all hope is lost for pet owners whose dog has tracheal collapse.
Intraluminal Tracheal Stenting
Although this does not involve opening an incision on the dog’s neck, it is considered a surgical procedure. It consists of using fluoroscopy to align and position the nickel-titanium mesh into the tracheal tube.
Fluoroscopy is basically a live feed of an X-ray machine and is very useful for diagnosing tracheal collapses. The nickel-titanium mesh is the same shape as the trachea, meaning the inner part is hollow.
Although tracheal stents most often cause quick amelioration of symptoms, post-operative complications present a serious problem. Because the neck is mobile and conditions the stent and trachea to move with it, the mesh can break and pierce the trachea.
Coughing might continue to be a problem because the tissue will grow over the mesh and cause irritation, just like a wound that is healing. Tissue overgrowth can lead to tracheal wall thickening, which will cause a problem similar to the collapse that was treated with it.
Medicines such as corticosteroids, analgesics, and, optionally, antibiotics will be necessary. Additionally, secondary care provided at home is a must and should not be taken lightly.
If you suspect your dog is not recovering from the surgical procedure, and the symptoms are becoming more pronounced or stagnate, you could ask your vet when to euthanize a dog with tracheal collapse for an answer based on medical facts alone.
Home Treatment Options

Fortunately, pet owners are not completely helpless when it comes to managing symptoms with quite a few things that are easy to do. After all, we would do anything to avoid further shortening our dog’s lifespan.
Weight Loss And Diet
I would say that the most important thing for symptom management at home is weight loss for dogs suffering from obesity. We already saw that this is one of the conditions that can increase the chance of a tracheal collapse, so weight management and dieting are key.
Considering the symptoms include difficulty breathing, exercise intolerance, and coughing, diet changes could prove to be more difficult than anticipated. While medical treatment is necessary for initial symptom inhibition, a healthy, low-fat, and low-carb diet is essential at home.
The drastically reduced physical activity will easily cause your dog to gain weight, even if it can barely eat from the coughing. Hydration is important because coughing every day all day is taxing on the body.
Swallowing hard foods can be challenging for dogs that have a tracheal collapse managed only by medication. This goes for dogs that recently underwent one of the surgical procedures. This is why changing from dry solid foods to soft foods is not a bad idea.
Make sure you have a lengthy discussion with your veterinarian before making any major changes in your dog’s diet. The surgeon will most likely have a list of foods that the dog can eat and switch to at one point in time.
People often suggest feeding your dog beef trachea due to the levels of chondroitin in it, but supplements have higher concentrations and are easier to digest for a dog with tracheal collapse.
Since neither chondroitin nor glucosamine is found in natural foods (in the amounts necessary for this condition), your veterinarian will give you a prescription for supplements that aid healing and cartilage growth in addition to lowering arthritis-induced pain.
Air Quality And Physical Activity
Clean air is important for reducing the immune system’s response that triggers coughing. Exposure to cigarette smoke, humid or dry air, or poor air quality, in general, will make the symptoms worse. Make sure these environmental factors are removed.
Dogs that suffer from tracheal collapse commonly have severe allergies to dust and dust mites. Other seasonal factors, such as tree, grass, and weed pollens, can aggravate the symptoms of your dog.
Make sure to use a humidifier if the dog has its bed positioned by a heating source like a radiator or heater. The air can get really dry with the direct source of heat, and it can further hamper the dog’s ability to lower its body temperature by expelling moisture through its mouth.
Senior dogs will have a harder time moving around, especially during the initial recovery period, so ease that for them by creating ramps to get up the couch and moving their bed (or yours) to the ground floor to rule out stairs as a nuisance.
This ailment is difficult for young, energetic dogs, and talking walks on a leash can be daunting. Replace your leash with a dog harness to avoid putting any pressure on the neck area around the trachea. Here are some of our favorite harnesses for a few dog breeds of different sizes:
- 6 best harnesses for Cane Corso
- 12 best harnesses for the Pitbull
- 12 best Yorkie harnesses
- 14 best harnesses for Dachshunds
How Long Can A Dog Live With Tracheal Collapse?

The average life expectancy depends on when the diagnosis was made, what grade the tracheal collapse is or was in, and what type of treatment the dog had.
Grades one and two of tracheal collapse can be successfully managed with medication until reaching grades three and four. A dog with a collapsed trachea has to be immediately hospitalized to avoid a fatal outcome within a few days or weeks.
Tracheal stenting usually means the dog has around two years of life after the stent is placed, but there are many cases where dogs lived more than four years after the procedure.
Post-operative complications present the biggest danger for a moderate life expectancy. Extraluminal prostheses have a somewhat shorter life expectancy due to the procedure having more points at which complications can occur.
Dogs that have bronchial collapse or larynx collapse at the same time or after surgery have a negative prognosis. While surgery for those two conditions exists, it is highly unlikely a dog would survive three separate procedures that have high chances of complications.
If everything goes according to the book, you are looking at three more years of life with your dog before things become unmanageable, thus leading to an answer to the dilemma when to euthanize a dog with tracheal collapse.
Conclusion
I remember when the family dog I grew up with had to be euthanized. It was raining, and the cold was frosting the street. I was riding my bicycle when my father called me and told me he had called a vet.
His voice was shaky, and I had never witnessed my father be that close to crying in my entire life. I turned my bicycle around and blankly stared at the car lights as I waited to cross the street for seven eternities and back.
By the time I came home, the injection had already started to fade my dog’s eyes. His last look was toward my father, whose shirt was now soaked in tears. This look was one of thankfulness, not of panic or fear.
He had been sick for weeks at that point, and making the right decision was the only thing left. When to euthanize a dog with tracheal collapse? Your dog’s eyes will answer that for you.
